 At her follow-up clinic visit, the patient’s mother reports that her daughter remains asymptomatic from a cardiovascular standpoint, and her pacemaker interrogation revealed that the device was working properly with low thresholds and pacing approximately 30% of the time. She was discharged home with the pacemaker programmed VVI with a rate of 90 beats per minute and hysteresis set at 60 beats per minute. 
She had significant oral aversion and feeding issues both preoperatively and postoperatively, which necessitated the prolonged postoperative course no active cardiac issues were present in the postoperative period. The patient tolerated the procedure well and was discharged from the hospital 14 days later. Additionally, she has received an extensive metabolic and genetic workup both in the past and during the current hospitalization that included a chromosomal analysis, DNA methylation studies, mitochondrial DNA, serum amino acids, urine organic acids, carnitine profile, long-chain fatty acid analysis, ammonia level, and a muscle biopsy, all of which were nondiagnostic.Īfter extensive discussions with the family, the decision was made to place an epicardial single-chambered pacemaker, which she underwent on hospital day 21. A barium swallow/upper gastrointestinal tract radiography revealed normal intestinal anatomy. A pH probe revealed only minimal gastroesophageal reflux, for which she was treated with ranitidine. An EEG showed slow background activity, but no lateralized, epileptiform, or electrographic seizures. A head magnetic resonance inage (MRI) showed diffuse volume loss above the tentorium and a watershed pattern of injury consistent with a history of hypotension. A transthoracic echocardiogram revealed normal intracardiac anatomy and good biventricular function, with a shortening fraction of 38%. On the Holter monitor, the heart rate ranged from 40 to 190 beats per minute, with an average heart rate of 130 beats per minute. A 24-h Holter monitor showed normal sinus rhythm with occasional sinus bradycardia and sinus pauses up to 3 s in duration with junctional escape. A 15-lead electrocardiogram showed normal sinus rhythm with a nonspecific T-wave abnormality, a QRS duration of 60 ms, a QT interval of 284 ms, and a QTc interval of 424 ms. The patient underwent an extensive workup. The majority of these pauses occurred when the patient was asleep, but she did have episodes while awake as well. Although some episodes were followed by junctional escape beats, others resolved with a sinus beat. Of note, these pauses would resolve spontaneously, and the patient never had any documented hemodynamic changes during the pauses, although an arterial line was never placed for invasive monitoring of her blood pressure. She continued to have sinus pauses, with a maximal duration of 15 s (Fig. She was weaned from the ventilator and extubated on hospital day 4. In the ICU, the patient was empirically started on antibiotics after cultures were drawn, but she required no other pharmacological support. The patient was intubated and transferred to the pediatric intensive care unit (ICU). During the pauses, she was given Epinephrine and Atropine, both of which transiently increased her heart rate from the 50s to greater than 100, but several minutes later, she would have recurrence of the sinus pauses. She did, however, have intermittent pauses on the monitor that lasted several seconds, but her perfusion was not compromised during these pauses. The patient was not being monitored at the time of arrest, and by the time monitors were connected, the patient had regained a pulse and was in sinus rhythm on the monitor. Her nurse initiated CPR after noting the patient to be apneic and pulseless. On hospital day 2, her mother reported that she suddenly became blue and began shaking. In March of 2005 she was admitted to our institution with acute gastroenteritis and dehydration. The patient’s family moved to the United States approximately 5 months prior to admission. She has always had poor oral intake, slow weight gain, nystagmus, and severe developmental delay. At that time, her mother reports that she had “funny heart beats” that were evaluated and the family was told there was nothing further to be done for the arrhythmia. At 2 months of age, she was hospitalized in Puerto Rico for viral meningitis. Her parents are first cousins and there is a strong family history of developmental delay but no family history of cardiac anomalies or arrhythmias.  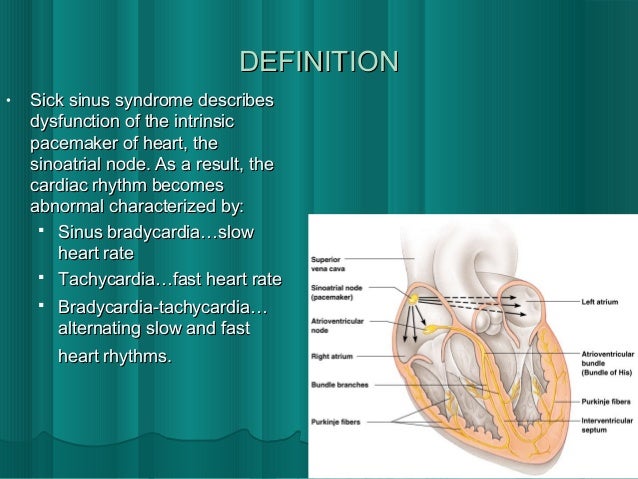
She remained hospitalized for 8 days after birth for hypotonia and poor feeding. 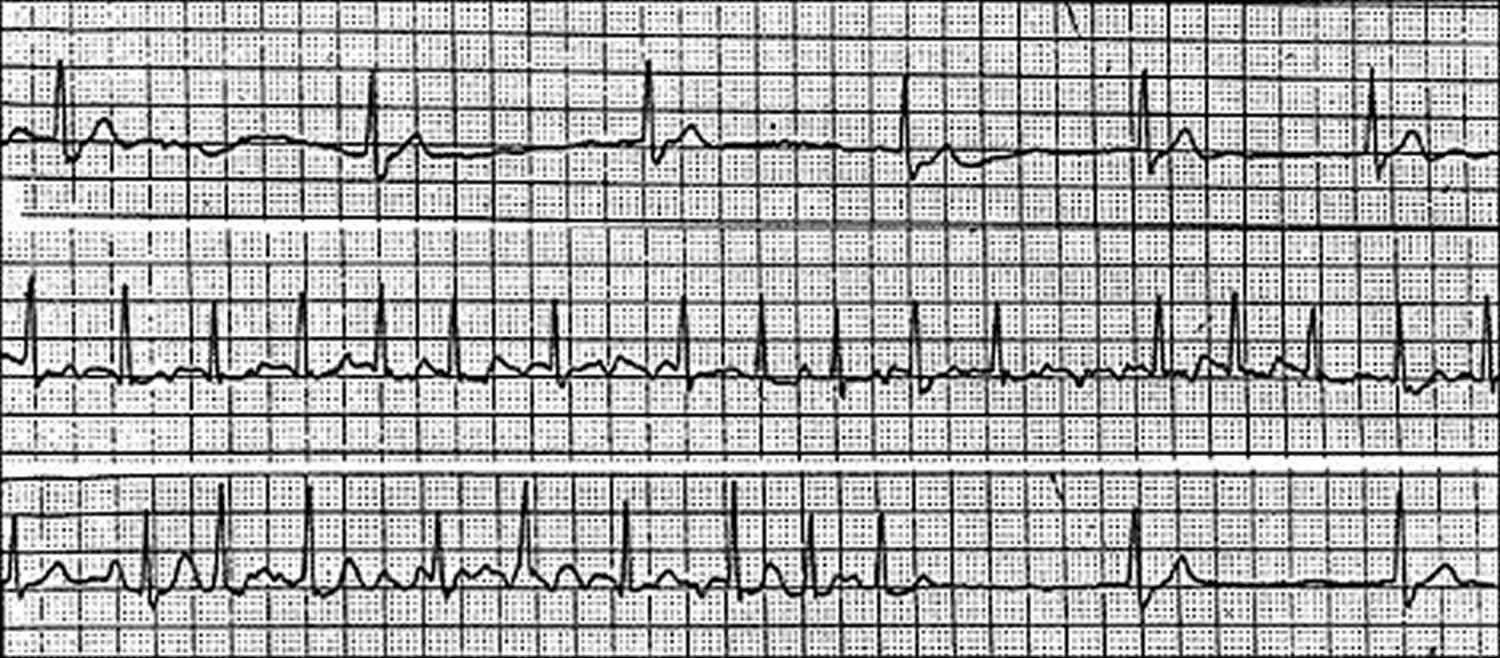
SJ is a 10-month-old girl who was the product of a full-term, uncomplicated pregnancy in Puerto Rico. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
